Doherty M. Treat-to-target urate-lowering therapy: the cornerstone of gout management. Practitioner October 2022;266(1862):11-15
Treat-to-target urate-lowering therapy: the cornerstone of gout management
25 Oct 2022
AUTHORS
Professor Michael Doherty MA MD FRCP FHEA, Emeritus Professor of Rheumatology, School of Medicine, University of Nottingham, Nottingham, UK
Competing interests: None
Article
Gout is a common complex disorder resulting from variable interaction between genetic, constitutional, and environmental factors. It is the most common inflammatory arthritis and has become more common in recent decades mainly due to increased longevity and the rising prevalence of obesity and metabolic syndrome. Urate is the end product of purine metabolism, and elevated serum urate (SU) results from increased production or reduced excretion. Increased production from endogenous purines mainly occurs because of overweight or obesity, but SU can also rise temporarily through excessive intake of purine-rich foods, fizzy drinks, beer or spirits. However, obesity is a far more important risk factor for gout than individual dietary elements. Heritability of gout is around 60%, and individual dietary factors account for < 1% of SU variance compared with 24% from the genetic variations currently identified. The most common presentation is a gout flare, characterised by acute onset of one or occasionally more hot, red, swollen joints which are extremely painful. In typical cases, clinical assessment alone is sufficient for diagnosis. An acute peripheral inflammatory monoarthritis that peaks within 24 hours, causing severe pain, and which subsequently resolves completely within 1-2 weeks is virtually pathognomonic of crystal synovitis. In chronic disease, asymmetrical polyarticular arthritis may be apparent, with or without tophi. Treat-to-target urate-lowering therapy (ULT) aims to reduce and maintain urate levels in peripheral joint tissues well below saturation (SU < 360 µmol/L). This prevents further crystal formation and gradually dissolves away existing crystals, after which no further flares occur, and further risk of crystal-induced joint damage is removed. Patients should be referred to rheumatology if: the diagnosis of gout is uncertain; gout treatment is not tolerated, contraindicated, or ineffective; the patient has CKD stages 3b to 5 (GFR categories G3b to G5); or the patient has had an organ transplant.
Gout is a common complex disorder resulting from variable interaction between genetic, constitutional, and environmental factors.
It is the most common inflammatory arthritis and has become more common in recent decades.1 The adult prevalence rose from 1.5% in 1997 to 2.5% in 2012, in the UK,2 and subsequently has remained at a similar stable level (2.3% in 2019).3 This increase is attributed mainly to increased longevity and the rising prevalence of obesity and metabolic syndrome.
The incidence is higher in men than women, in a ratio of 4:1, and increases with age, resulting in 15% of men and 6% of women aged 80-84 years, in the UK, being affected in 2019.2
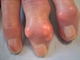
Apart from very painful disease flares, gout can also cause damage to joints with resulting chronic usage-related pain; increased likelihood of the patient needing knee or hip joint replacement, even if the individual has not experienced flares in those joints;4 tophi, disfiguring subcutaneous nodules (see figure 1); and reduced quality of life.5
Furthermore, elevated serum urate (SU), which is acidic, together with chronically raised serum inflammatory markers (reflecting subclinical crystal inflammation) that occur in people with hyperuricaemia and gout may damage vascular endothelium and predispose to cardiovascular disease (CVD) and chronic kidney disease (CKD).6,7 Gout is also associated with other comorbidities (e.g. nephrolithiasis, metabolic syndrome, malignancy, liver disease),8 and increased mortality.8
Treat-to-target urate-lowering therapy (ULT) combined with effective patient education can eliminate the urate crystals that cause gout.9,10 However, gout management remains suboptimal in the UK.2,11 Although 40% of patients at diagnosis appear eligible for ULT as they have ‘severe’ gout (i.e. frequent flares, joint damage, tophi, CKD, nephrolithiasis) and 85% become eligible within five years, less than half ever receive ULT.12 Furthermore, when ULT is prescribed it is generally at a fixed dose without titration to a target SU level, and adherence is very poor.12,13 In 2021, 40% of people with gout in the UK were receiving ULT, but only 30% of those achieved the target SU, meaning that overall, only 12% of gout patients are on potentially curative treatment.14
Suboptimal management largely reflects misconceptions among both patients and healthcare professionals. Common misconceptions are that gout is different from ‘arthritis’, and that it is self-induced by poor lifestyle i.e. overindulgence in food and alcohol, and women often perceive it as a man’s disease.15,16 Therefore, education is pivotal in gout management. These common misconceptions may delay patients seeking advice until gout is well established.
Causes
Gout is caused by precipitation of monosodium urate crystals in and around joints when the urate level exceeds saturation (indicated by an SU > 360 µmol/L or 6 mg/dl).17-20 Urate crystals preferentially form in peripheral, cooler joints, especially those with osteoarthritis (OA); changes in osteoarthritic cartilage facilitate crystal formation.17,18 Crystal deposition builds up slowly over years without causing symptoms.19,20 Eventually, crystal shedding may occur where some crystals on the cartilage surface spill into the joint cavity and are recognised as foreign bodies by the innate immune response, triggering intense synovitis i.e. a gout flare.6,19,20 Also, continuing slow build-up of condensed crystal deposits, microtophi, in cartilage and subchondral bone may damage joints and eventually cause symptoms and signs resembling OA.18-20
Urate is the end product of purine metabolism, and elevated SU results from increased production or reduced excretion.20 Endogenous purines are the main source of urate. Increased production from endogenous purines mainly occurs because of overweight or obesity. SU levels can also rise temporarily as a result of excessive intake of purine-rich foods, e.g. red meat, seafood, or fructose, which is present in many fizzy drinks and influences hepatic urate release, beer and spirits.17,19,20 However, obesity is a far more important risk factor for gout than dietary constituents.20,21 Urate is predominantly excreted through the kidneys and the heritable component of gout is now known to result predominantly from inefficient urate excretion.19-21 Oestrogen increases renal urate excretion, so until the menopause women have lower SU levels than men.20 In addition, CKD, metabolic syndrome, and drugs that affect renal function, e.g. thiazide diuretics, beta-blockers, ACE inhibitors, all reduce urate elimination.20
In twin studies heritability of gout is around 60% and recent studies show that individual dietary factors account for < 1% of SU variance compared with 24% from the genetic variations currently identified so far.21
Presentation
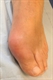
The most common presentation is a gout flare, characterised by acute onset of one, and occasionally more, hot, red, swollen joints which are extremely painful and very tender.22 Peak severity of flares occurs in 12-24 hours. Most flares affect the feet, knees, hands or elbows, although any joint can be affected. Involvement of the first metatarsophalangeal joint, podagra, is very characteristic, see figure 2.22
Insidious onset of chronic usage-related joint pain, especially in joints already affected by OA, e.g. finger interphalangeal joints with nodal OA, is a less common presentation.
Patients may also present with subcutaneous tophi, especially older people. Tophi particularly occur on extensor surfaces of toes, fingers, heels, knees and elbows, appearing as nodules with heterogeneous consistency (unlike homogeneous rheumatoid nodules), sometimes with white-yellow discoloration – urate crystals are white. Patients may report previous gout flares but some present just with tophi or chronic joint symptoms.
Confirming diagnosis
Clinical assessment alone is generally sufficient for diagnosis.22 An acute peripheral inflammatory monoarthritis that peaks within 24 hours, causing very severe pain, and which subsequently resolves completely within 1-2 weeks is virtually pathognomonic of crystal synovitis. Involvement of the first metatarsophalangeal joint is highly characteristic of gout. The patient may have risk factors, such as a family history of gout, obesity, hypertension, renal impairment, or diuretic and antihypertensive drug treatment.
During a flare clinical examination will reveal an extremely tender, hot swollen joint which may be red, often with adjacent periarticular soft tissue swelling. In patients with chronic disease, asymmetrical polyarticular arthritis may be apparent, with or without tophi.
A raised SU level helps confirm the diagnosis, though SU levels may be normal during a flare because SU levels fall during acute inflammation. If gout is suspected but the SU is < 360 µmol/L, the blood test should be repeated at least two weeks after the attack has resolved.22
If the joint can be aspirated, presence of synovial fluid urate crystals on microscopy confirms the diagnosis with 100% confidence (see figure 3).23
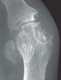
Usually, radiographs do not show characteristic features of gout until late in the disease (see figure 4, p13). However, joint ultrasound readily demonstrates characteristic features (microtophi in synovium and periarticular sites, crystal deposits in superficial articular cartilage producing a parallel double contour sign aligned with subchondral bone, and bone erosions) at first presentation in multiple peripheral sites, not just the presenting symptomatic joint.24 Dual energy computed tomography (DECT) can also identify urate crystal deposits but is less widely available than ultrasonography.
It is particularly useful in diagnosing uncommon axial gout.
Differential diagnosis
The main differential diagnosis is acute calcium pyrophosphate crystal arthritis which is also associated with OA. However, it is less common than gout, mainly affects those aged over 60, and tends to target the knee. Septic arthritis is far less common than gout and usually presents as monoarthritis, most often of the knee. The onset is slower with symptoms and signs getting progressively worse over several days rather than just hours, and it is often associated with fever and systemic upset.
Diagnosis of gout should lead to consideration of, and screening for, associated comorbidity e.g. hypertension, hyperlipidaemia, diabetes, CKD.22
Management
NICE published its first gout guideline in June 2022,22 this aligns well with the 2016 British Society for Rheumatology (BSR) guideline which was endorsed by NICE.23 The following management advice incorporates the key NICE recommendations.
Gout flares
Flares are extremely painful and need rapid treatment. Treatment should be started as soon as possible after the first symptoms appear.23 All patients should be advised to rest the joint23 and apply ice packs locally.22,23
NICE recommends either an NSAID, colchicine, or a short course of oral corticosteroids as first-line oral treatments, taking into account comorbidities, co-prescriptions and patient preferences.22 NSAIDs (including selective COX-2 inhibitors) should be given at maximal doses but should be used with caution in people with renal impairment or CVD.22,23 A proton pump inhibitor (PPI) should be prescribed with the NSAID in older patients, and in those with comorbidities or increased gastrointestinal risk.22,23 There is no evidence for superiority of one NSAID over another.23
Although colchicine is not an analgesic, if it is started within the first 12-24 hours of the flare it can reduce crystal-induced triggering of the innate immune (inflammasome) response.
It can be started at 0.5 mg twice daily and increased, if tolerated, to three times daily and then to a maximum of four times daily.23 Do not exceed a maximum of 6 mg per course, and do not repeat a course within three days. Such dosing minimises the risk of side effects, especially diarrhoea which is common at higher doses.23,25 An alternative regimen is a 1 mg loading dose followed one hour later by 0.5 mg for the first day, and subsequently 0.5 mg two to four times daily depending on tolerability.25
With renal impairment the dose should be reduced to 0.5 mg daily. Colchicine interacts with cytochrome P450 3A4 inhibitors (e.g. ciclosporin, ketoconazole, clarithromycin, erythromycin, verapamil, diltiazem)23 so should be used with caution in people taking these drugs. Statins should be stopped temporarily while patients are being treated with colchicine.23
A short course of oral corticosteroids, e.g. prednisolone 35 mg daily,26 is particularly useful in people with contraindications or intolerance to NSAIDs or colchicine. It is the best option for older people with multiple comorbidities.23
Intramuscular corticosteroid injection (e.g. triamcinolone 40-60 mg) is an alternative.22 Joint aspiration and injection of long-acting corticosteroids, e.g. methylprednisolone acetate or triamcinolone acetonide, provides rapid relief and usually aborts the flare.23 However, this option is often impractical in primary care.22
Long-term treatment
Long-term treatment aims to eliminate urate crystals and gout by reducing and maintaining urate levels in peripheral joint tissues well below saturation (SU < 360 μmol/L). This prevents further crystal formation and gradually dissolves existing crystals, after which no further flares occur, and further risk of crystal-induced joint damage is removed. The lower the SU the faster the crystals dissolve and the sooner the gout resolves.23 The minimum target SU is < 360 μmol/L, though a lower target of < 300 μmol/L, at least for the first 2-4 years, is recommended for people with tophi and joint damage, or who still have frequent flares after achieving the < 360 μmol/L target.22,23 There is also growing evidence that reducing SU to target may benefit associated comorbidities, including CVD and CKD, that link pathogenically with elevated urate and raised serum inflammatory markers.19,23 Therefore, treat-to-target ULT may have additional health benefits.
Providing individualised patient information about gout (its risk factors, associations, possible outcomes, and available treatment strategies), exploring the patient’s perceptions about the condition, and involving the patient in shared decision making are all central to achieving this target and maintaining ULT adherence.9,10,22,23,27
The optimal time for patient education and engagement is once any flare has settled and the patient can fully focus on understanding gout and its treatment. Online information and patient leaflets, can be used to support this process (see External weblinks).
Advice on lifestyle modification should be tailored to individual needs. Where appropriate, patients should be encouraged to lose weight if overweight, and reduce excessive intake of high-purine foods such as red meat, offal, and seafood, beer, spirits and fructose-rich drinks.22,23 Episodes of excessive alcohol and purine-rich food intake may help provoke gout flares by facilitating recognition of the crystals by the innate immune system but have little or no effect on urate crystal formation.6 NICE has concluded that there is insufficient evidence to advise a specific diet or exclusion of individual dietary items.22
In patients with hypertension, losartan and calcium channel blockers, which are uricosuric and lower SU, can be used in preference to beta-blockers, diuretics, ACE inhibitors and non-losartan angiotensin II receptor blockers, which elevate SU by reducing renal excretion.28
Even when there are modifiable risk factors that are addressed successfully, this usually does not lower SU to the target level;23 almost all patients require ULT.23,29 Although traditionally reserved for patients with ‘severe’ gout (e.g. those having several flares/year, tophi, joint damage, CKD, nephrolithiasis), NICE and other recent rheumatology guidelines agree that ULT should be discussed with all patients with gout as part of full education around the time of first diagnosis,22,23,29 and initiated following first presentation to reduce the long-term complications associated with gout.23,29 This aligns with more definitive treatment approaches used for other chronic inflammatory diseases, and recognition of gout as a potentially serious health condition. When fully informed, almost all patients wish to receive ULT, and subsequent adherence is excellent.9,27
NICE recommends either allopurinol or febuxostat as equal first-line ULTs, with allopurinol being offered first to people with major CVD.22 If the first is unsuccessful the other should be tried. Both are xanthine oxidase inhibitors that reduce urate production. The usual starting dose of allopurinol is 100 mg, which is then up-titrated to a maximum of 900 mg daily against the SU level by 100 mg increments every four weeks until the target SU of < 360 μmol/L or < 300 μmol/L is achieved.22,23, 29 Such slow up-titration reduces the risk of severe upset, as well as possible provocation of flares associated with rapid drops in SU. Recent UK studies report 400-500 mg/day as the average dose required to achieve target9,27 which is higher than the 100-300 mg/day range usually prescribed in general practice.12,14
Oxypurinol, the active metabolite of allopurinol, is excreted via the kidneys so lower doses of allopurinol (initially 50 mg/day with subsequent 50 mg increments) should be used in those with marked renal impairment.22,23
In patients who are also on warfarin, slow up-titration with regular INR checks is required because of competitive protein-binding, and occasionally the warfarin dose will need to be reduced. Most patients tolerate allopurinol, but around one in ten develop troublesome GI symptoms or a rash that requires cessation of treatment. A rare serious reaction, presenting as DRESS (drug reaction or rash with eosinophilia and systemic symptoms) may develop, but this usually occurs in patients with CKD who have been started on too high a dose (e.g. 300 mg), so is largely avoidable.
Febuxostat is a newer ULT (now generic) which mainly undergoes hepatic metabolism, so no dose reduction is required with renal impairment. Tolerability and side-effect profile are similar to those of allopurinol, including rare DRESS syndrome, but there are unconfirmed reservations over its cardiovascular safety.22,23 It is available in just two doses (80 mg and 120 mg daily), so there is only one option for up-titration four weeks after initiation. This allows the target SU to be reached rapidly and with less monitoring than with allopurinol,22 but such rapid lowering of SU is more likely to provoke flares.
ULT adherence may be compromised if patients are not aware of the potential risk of increased flare rates following ULT initiation, possibly caused by partial dissolution and reduction in size of crystals which facilitates crystal shedding into the joint.
NICE recommends consideration of prophylaxis to reduce flare frequency in the first months of ULT initiation, using low-dose colchicine (0.5 mg twice daily).22 If this is contraindicated, not tolerated or ineffective, a low dose of oral NSAID or corticosteroid are alternatives.22 These may be taken with a PPI, depending on the patient’s individual risk factors for adverse events.22
There is a stronger case for prophylaxis with febuxostat, but whether slow up-titration of allopurinol causes a significant risk of additional flares remains controversial. Once fully informed and involved in decision making, most patients prefer to manage flares as required rather than take prophylactic medications in addition to their new ULT.9,27
Uricosuric drugs (benzbromarone, probenecid and sulfinpyrazone) are alternative ULTs but these have limited availability, are contraindicated in significant renal impairment, and are mainly prescribed in secondary care.
Monitoring and follow-up in primary care
Once the target SU is achieved, NICE recommends subsequent annual monitoring to ensure SU is maintained on target.22 Patients may continue to experience flares during the first two or three years of successful ULT, but provided the target SU is maintained, gout flares eventually cease, any subcutaneous tophi resolve, and quality of life is enhanced.19,20,29 Once clinically improved, people with severe gout who initially were given the lower target of < 300 μmol/L, to speed up dissolution of existing crystals, can change to the long-term higher target of < 360 μmol/L to prevent new crystal formation.23,29
Referral
NICE22 recommends considering referral to a rheumatology service if:
• The diagnosis of gout is uncertain
• Gout treatment is contraindicated, not tolerated or ineffective
• The patient has CKD stages 3b to 5 (GFR categories G3b to G5)
• The patient has had an organ transplant
A 2018 community-based randomised controlled trial, involving 517 patients, compared nurse-led care, involving full patient education and engagement and a treat-to-target ULT strategy i.e. NICE recommended best practice,22 with usual GP-led care over a two-year period.27 At two years nurse-led care resulted in very high uptake (96%) and excellent adherence to ULT; achievement of SU < 360 μmol/L in 95% and < 300 μmol/L in 84%; significant reductions in flare frequency and tophi; and improved quality of life. Many patients had comorbidities and more than 20% had CKD stage 3 or higher. Compared with usual care, this model was cost effective at two years and estimated to be cost saving at five years. Such results highlight the importance and success of recommended individualised education and treat-to-target ULT, principles that should be applied by any healthcare professional managing people with gout.27
Conclusion
Gout is the only common chronic arthritis in which the pathogenic agent (urate crystals) can be eliminated. In primary care this can be achieved in more than 9 out of 10 patients through effective patient education and engagement and a treat-to-target ULT strategy.
REFERENCES
1 Kuo CF, Grainge MJ, Zhang W et al. Global epidemiology of gout: prevalence, incidence and risk factors. Nat Rev Rheumatol 2015;11:649-62
2 Kuo CF, Grainge MJ, Mallen C et al. Rising burden of gout in the UK but continuing suboptimal management: a nationwide population study. Ann Rheum Dis 2015;74:661-67
3 Abhishek A, Tata LJ, Mamas M et al. Has the gout epidemic peaked in the UK? A nationwide cohort study using data from the Clinical Practice Research Datalink, from 1997 to across the COVID-19 pandemic in 2021. Ann Rheum Dis 2021;81:898-99
4 Kuo CF, Chou IJ, See LC et al. Urate-lowering treatment and risk of total joint replacement in patients with gout. Rheumatology 2018;57:2129-39
5 Chandratre P, Roddy E, Clarson L et al. Health-related quality of life in gout: a systematic review. Rheumatology 2013;52(11):2031-40
6 Joosten LAB, Crişan TO, Bjornstad P, et al. Asymptomatic hyperuricaemia: a silent activator of the innate immune system. Nat Rev Rheum 2020;16:75-86
7 Luis-Rodriguez D, Donate-Correa J, Martin-Nunez E et al. Serum urate is related to subclinical inflammation in asymptomatic hyperuricaemia. Rheumatology 2021;60:371-79
8 Kuo CF, Grainge MJ, Mallen C et al. Comorbidities in patients with gout prior to and following diagnosis: case-control study. Ann Rheum Dis 2016;75:210-17
9 Rees F, Jenkins W, Doherty M. Patients with gout adhere to curative treatment if informed appropriately: proof-of-concept observational study. Ann Rheum Dis 2013;72(6):826-30
10 Rees F, Hui M, Doherty M. Optimizing current treatment of gout. Nat Rev Rheumatol 2014;10(5):271-83
11 Cottrell E, Crabtree V, Edwards JJ et al. Improvement in the management of gout is vital and overdue: an audit from a UK primary care medical practice. BMC Fam Pract 2013;14:170
12 Kuo CF, Grainge M, Mallen C et al. Eligibility for and prescription of urate-lowering treatment in incident gout patients in England. JAMA 2014;312:2684-86
13 Scheepers LEJM, Burden AM, Arts ICW et al. Medication adherence among gout patients initiated allopurinol: a retrospective cohort study in the Clinical Practice Research Datalink (CPRD). Rheumatology 2018;57:1641-50
14 Abhishek A, Cipolletta E, Nakafero G et al. Serum urate outcomes of treat-to-target urate lowering treatment: results of a nationwide cohort study from 1997 to the COVID-19 pandemic using data from the Clinical Practice Research Datalink. Ann Rheum Dis 2022 Jun 30; annrheumdis-2022-222668 Online ahead of print
15 Spencer K, Carr A, Doherty M. Patient and provider barriers to effective management of gout in general practice: a qualitative study. Ann Rheum Dis 2012;71(9):1490-95
16 Doherty M, Jansen TL, Nuki G et al. Gout: why is this curable disease so seldom cured? Ann Rheum Dis 2012;71:1765-70
17 Chhana A, Lee G, Dalbeth N. Factors influencing the crystallization of monosodium urate: a systematic literature review. BMC Musculoskelet Disord 2015;16:296
18 Towiwat P, Chhana A, Dalbeth N. The anatomical pathology of gout: a systematic literature review. BMC Musculoskelet Disord 2019;20:140
19 Sivera F, Andres M, Dalbeth N. A glance into the future of gout. Ther Adv Musculoskelet Dis 2022;14: 1759720X221114098
20 Perez-Ruiz F, Dalbeth N, Bardin T. A review of uric acid, crystal deposition disease, and gout. Adv Ther 2015;32:31-41
21 Major TJ, Topless RK, Dalbeth N et al. Evaluation of the diet wide contribution to serum urate levels; meta-analysis of population based cohorts. BMJ 2018;363: k3951
22 National Institute for Health and Care Excellence. NG219. Gout diagnosis and management. NICE. London. 2022 www.nice.org.uk/guidance/ng219
23 Hui M, Carr A, Cameron S et al. The British Society for Rheumatology guideline for the management of gout. Rheumatology 2017;56(7):1056-59
24 Stewart S, Maxwell H, Dalbeth N. Prevalence and discrimination of OMERACT-defined elementary ultrasound lesions of gout in people with asymptomatic hyperuricaemia: a systematic review and meta-analysis. Sem Arthritis Rheum 2019;49:62-73
25 Terkeltaub RA, Furst DE, Bennett K et al. High versus low dosing of oral colchicine for early acute gout flare: Twenty-four-hour outcome of the first multicenter, randomized, double-blind, placebo-controlled, parallel-group, dose-comparison colchicine study. Arthritis Rheum 2010;62(4):1060-68
26 Janssens HJ, Janssen M, van de Lisdonk EH et al. Use of oral prednisolone or naproxen for the treatment of gout arthritis: a double-blind, randomised equivalence trial. Lancet 2008;371:1854-60
27 Doherty M, Jenkins W, Richardson H, et al. Efficacy and cost-effectiveness of nurse-led care involving education and engagement of patients and a treat-to-target urate-lowering strategy versus usual care for gout: a randomised controlled trial. Lancet 2018;392:1403-12
28 Choi HK, Soriano LC, Zhang Y et al. Antihypertensive drugs and risk of incident gout among patients with hypertension: population based case-control study. BMJ 2012;344:d8190
29 Richette P, Doherty M, Pascual E et al. 2016 updated EULAR evidence-based recommendations for the management of gout. Ann Rheum Dis 2017;76:29-42
ARTICLE IN PDF
EXTERNAL WEBLINKS
For patients

 = Registered users
= Registered users = Paid-up subscribers
= Paid-up subscribers